On November 5, 2025, the Centers for Medicare & Medicaid Services (CMS) released the 2026 Medicare Physician Fee Schedule (PFS) Final Rule. This rule outlines updates to the Quality Payment Program (QPP), including key changes to the Merit-based Incentive Payment System (MIPS), Alternative Payment Models (APMs), and related reporting requirements for the 2026 performance year. Below is a summary of key policy updates, along with all major requirements for the 2026 MIPS performance period affecting eligible clinicians and groups.
MIPS Eligibility & Participation Overview
What’s New for 2026?
There are no changes to MIPS eligibility criteria or participation options for the performance year.
Who is Eligible?
Clinicians are required to participate in MIPS if they:
- Belong to a MIPS-eligible clinician type
- Exceed all three elements of the low-volume threshold during both segments of the MIPS Determination Period:
- Bill more than $90,000 in Medicare Part B allowed charges for covered professional services; and
- Provide covered professional services to more than 200 Medicare Part B beneficiaries; and
- Furnish more than 200 covered professional services to Medicare Part B beneficiaries.
Determination Periods
CMS assesses eligibility using two 12-month segments:
- Segment 1: October 1, 2024 – September 30, 2025
- Segment 2: October 1, 2025 – September 30, 2026
Exemptions
Clinicians are excluded from MIPS if they:
- Are newly enrolled in Medicare during the performance period.
- Participate sufficiently in an Advanced Alternative Payment Model (APM) and are designated as Qualifying APM Participants (QPs).
- Do not exceed the low-volume threshold in either segment of the determination period.
How to Check Your Eligibility
Your initial 2026 MIPS eligibility status is available now. CMS will publish your final eligibility status in December. If you work at multiple practices, you may be required to report at one but not at another—eligibility is determined at the TIN/NPI level.
- Use the QPP Participation Status Tool
Reporting Options
There are several ways to participate in MIPS for the 2026 performance year. Choose the option that best fits your practice:
Traditional MIPS
Traditional MIPS is the original reporting pathway. Below is a summary of what is required for each performance category:
- Quality - Select 6 measures (including an Outcome or High Priority measure) and collect data for the full year (Jan 1–Dec 31). Review the quality measure benchmarks when selecting measures to understand how benchmarks affect scoring. You may also choose to report a complete specialty measure set as an alternative to selecting individual measures. In addition, CMS will automatically evaluate any applicable claims-based measures.
- Improvement Activities - Choose 2 activities and perform each for at least 90 continuous days. Some clinicians with special status only have to choose 1 activity.
- Promoting Interoperability measures - Report the complete measure set for a continuous 180-day period. Some clinicians with special status may not be required to report data for this performance category.
- Cost - No data submission required. CMS calculates your Cost performance category score based on claims.
MIPS Value Pathways (MVPs)
MVPs are a newer, more streamlined option tailored to specific specialties or conditions. Each MVP includes a focused set of:
- Quality measures - Select 4 measures within the MVP and collect data for the full year (Jan 1–Dec 31). CMS also evaluates a population health measure using claims data.
- Improvement Activities - Choose 1 activity within the MVP and perform it for at least 90 continuous days.
- Promoting Interoperability - Report the measure set for a continuous 180-day period. Some clinicians with special status may not be required to report data for this performance category.
- Cost measures - No data submission required. CMS scores you using MVP-specific cost measures.
MIPS APM Participants
The Alternative Payment Model (APM) Performance Pathway (APP) is a simplified reporting framework available to clinicians participating in a MIPS APM. It features a defined set of quality measures and is designed to reduce reporting burden, provide additional scoring opportunities, and promote greater participation in APMs.
Performance Threshold Remains at 75 Points
The MIPS performance threshold will remain at 75 points. Each clinician’s or group’s performance across the MIPS categories will be combined into a Final Score ranging from 0 to 100 points. This score is then compared to the 75-point threshold to determine whether a positive, neutral, or negative payment adjustment will apply. Payment adjustments based on performance will continue to range up to ±9%.
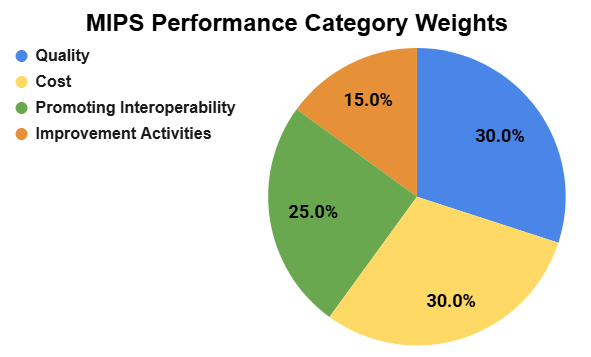
2026 Performance Category Weights
Understanding how each MIPS performance category contributes to your final score is essential for successful reporting. The chart below shows the percentage weight assigned to each category.
Small practices automatically receive reweighting for the Promoting Interoperability (PI) category. If a small practice does not submit PI data, the Quality category will be weighted at 40% and Improvement Activities at 30%.
MIPS Performance Category Weight Redistribution Policies
Depending on your practice size and reporting circumstances, CMS may reweight one or more performance categories. The tables below outline how performance category weights are adjusted for both large and small practices.
Large Practice Participants
The table below illustrates the performance category reweighting policies that CMS will apply to large practice participants (practice has 16 or more clinicians):
| Reweighting Scenario | Quality | Cost | Improvement Activities (IA) | Promoting Interoperability (PI) |
|---|---|---|---|---|
| No Reweighting Needed | ||||
| Scores for all 4 performance categories | 30% | 30% | 15% | 25% |
| Reweight 1 Performance Category | ||||
| No Cost | 55% | 0% | 15% | 30% |
| No PI | 55% | 30% | 15% | 0% |
| No Quality | 0% | 30% | 15% | 55% |
| No IA | 45% | 30% | 0% | 25% |
| Reweight 2 Performance Categories | ||||
| No Cost and no PI | 85% | 0% | 15% | 0% |
| No Cost and no Quality | 0% | 0% | 15% | 85% |
| No Cost and no IA | 70% | 0% | 0% | 30% |
| No PI and no Quality | 0% | 50% | 50% | 0% |
| No PI and no IA | 70% | 30% | 0% | 0% |
| No Quality and no IA | 0% | 30% | 0% | 70% |
Small Practice Participants
The table below illustrates the performance category reweighting policies that CMS will apply to small practice participants (practice has 15 or fewer clinicians):
| Reweighting Scenario | Quality | Cost | Improvement Activities (IA) | Promoting Interoperability (PI) |
|---|---|---|---|---|
| No Reweighting Needed | ||||
| Scores for all 4 performance categories | 30% | 30% | 15% | 25% |
| Reweight 1 Performance Category | ||||
| No Cost | 55% | 0% | 15% | 30% |
| No PI* | 40% | 30% | 30% | 0% |
| No Quality | 0% | 30% | 15% | 55% |
| No IA | 45% | 30% | 0% | 25% |
| Reweight 2 Performance Categories | ||||
| No Cost and no PI* | 50% | 0% | 50% | 0% |
| No Cost and no Quality | 0% | 0% | 15% | 85% |
| No Cost and no IA | 70% | 0% | 0% | 30% |
| No PI and no Quality | 0% | 50% | 50% | 0% |
| No PI and no IA | 70% | 30% | 0% | 0% |
| No Quality and no IA | 0% | 30% | 0% | 70% |
Quality Measure Inventory Changes
There are a total of 187 quality measures for the 2026 performance period which reflect:
- 5 new Quality measures
- Removal of 10 Quality measures
- Substantive changes to 30 existing Quality measures
A list of new measures, along with their collection types, is outlined in the table below.
A list of measures that have been removed or partially removed is outlined in the table below.
| Retired Quality Measures | Collection Type |
|---|---|
| #185 Colonoscopy Interval for Patients with a History of Adenomatous Polyps – Avoidance of Inappropriate Use | MIPS CQM |
| #264 Sentinel Lymph Node Biopsy for Invasive Breast Cancer | MIPS CQM |
| #290 Assessment of Mood Disorders and Psychosis for Patients with Parkinson's Disease | MIPS CQM |
| #322 Cardiac Stress Imaging Not Meeting Appropriate Use Criteria: Preoperative Evaluation in Low-Risk Surgery Patients | MIPS CQM |
| #419 Overuse of Imaging for the Evaluation of Primary Headache | MIPS CQM |
| #424 Perioperative Temperature Management | MIPS CQM |
| #443 Non-Recommended Cervical Cancer Screening in Adolescent Females | MIPS CQM |
| #487 Screening for Social Drivers of Health | MIPS CQM |
| #498 Connection to Community Service Provider | MIPS CQM |
| #508 Adult COVID-19 Vaccination Status | MIPS CQM |
CMS has removed “health equity” from the definition of high priority measures, narrowing the scope to core clinical domains such as outcomes, safety, and care coordination.
Quality Measure Benchmarks
When clinicians or groups submit measures for the quality performance category, their performance on each measure is compared against the measure's benchmark to determine how many points the measure earns. A clinician or group can receive anywhere from 1 to 10 points for each MIPS measure based on this comparison as long as the data completeness standards and case minimum requirements are met. When selecting measures to report, carefully review the 2026 benchmarks to understand how measures will be scored.
Flat Benchmarks for a Subset of Topped-Out Measures
A flat benchmarking methodology will be used for certain topped-out measures, specifically those within specialty sets that have limited options and a high number of topped-out measures, where there is a lack of new measure development. This approach aims to address challenges in meaningful MIPS participation in these areas. Each year, CMS will propose the specific measures to which this policy will apply and detail the corresponding benchmarks.
| Performance Rate | Available Points |
|---|---|
| 84-85.9% | 1-1.9 |
| 86-87.9% | 2- 2.9 |
| 88-89.9% | 3-3.9 |
| 90-91.9% | 4-4.9 |
| 92-93.9% | 5-5.9 |
| 94-95.9% | 6-6.9 |
| 96-97.9% | 7-7.9 |
| 98-99.9% | 8-8.9 |
| 99-99.99% | 9-9.9 |
| 100% | 10 |
Improvement Activities Category Updates
Improvement Activities Inventory
There are nearly 100 Improvement Activities to choose from this performance year. Updates to the Improvement Activities inventory reflect the following changes:
- 3 new activities
- Modification of 7 existing activities
- Removal of 8 activities, in addition to 4 previously scheduled for removal in 2026
- The “Achieving Health Equity” subcategory has been replaced with a new subcategory: “Advancing Health and Wellness”
| Improvement Activities Removed |
| IA_ AHE_5 MIPS Eligible Clinician Leadership in Clinical Trials or CBPR |
| IA_AHE_8 Create and Implement an Anti-Racism Plan |
| IA_AHE_9 Implement Food Insecurity and Nutrition Risk Identification and Treatment Protocols |
| IA_AHE_11 Create and Implement a Plan to Improve Care for Lesbian, Gay, Bisexual, Transgender, and Queer Patients |
| IA_AHE_12 Practice Improvements that Engage Community Resources to Address Drivers of Health |
| IA_BMH_8 Electronic Health Record Enhancements for BH Data Capture |
| IA_CC_1 Implementation of Use of Specialist Reports Back to Referring Clinician or Group to Close Referral Loop |
| IA_CC_2 Implementation of Improvements that Contribute to More Timely Communication of Test Results |
| IA_PM_26 Vaccine Achievement for Practice Staff: COVID-19, Influenza, and Hepatitis B |
| IA_PM_6 Use of Toolsets or Other Resources to Close Health and Health Care Inequities Across Communities |
| IA_PM_12 Population Empanelment |
| IA_ERP_3 COVID-19 Clinical Data Reporting with or without Clinical Trial |
Reporting Requirements by Participation Type
Traditional MIPS Reporting
Clinicians, groups, and virtual groups with any of the following special statuses:
- Small Practice
- Rural
- Non–Patient Facing
- Health Professional Shortage Area (HPSA)
→ Must attest to one improvement activity.
All other clinicians, groups, and virtual groups:
→ Must attest to two improvement activities.
MIPS Value Pathways (MVP) Reporting
All clinicians, groups, and subgroups (regardless of special status):
→Must attest to one improvement activity.
Promoting Interoperability (PI) Category Updates
CMS has made several technical updates to strengthen data security, modernize guidance, and add flexibility in response to real-world reporting challenges.
- The Security Risk Analysis measure will now require an additional attestation confirming that clinicians conducted risk management activities, as outlined under the HIPAA Security Rule.
- Clinicians will be required to use the updated 2025 SAFER Guides for their self-assessments under the High Priority Practices measure.
- The Public Health and Clinical Data Exchange objective has been modified by adopting a new optional bonus measure: the Public Health Reporting Using TEFCA measure. The measure is 1 of 4 available bonus measures under the Public Health and Clinical Data Exchange objective, in which a maximum of 5 points can be earned if reporting one, more than one, or all
optional bonus measures.
Automatic reweighting will continue to apply only to MIPS eligible clinicians, groups, and virtual groups with the following special statuses:
- Ambulatory Surgical Center (ASC)-based
- Hospital-based
- Non–Patient Facing
- Small Practice
Cost Category Updates
The Cost performance category remains largely unchanged in the 2026 final rule, but CMS has made refinements that aim to improve fairness and provide more transparency for future cost scoring.
- No new cost measures have been adopted, and none are being removed. The total number of cost measures remains at 35 for the 2026 performance year.
- CMS has updated the Total Per Capita Cost (TPCC) measure to limit instances where TPCC is attributed to highly specialized groups based solely on billing of advanced care practitioners.
- Looking ahead, CMS finalized a 2-year informational-only feedback period for any new cost measures finalized in future years. During this time, clinicians will see performance feedback without the measure contributing to their MIPS final score—giving practices time to understand and adapt before any financial impact.
MIPS Value Pathways (MVPs)
There are 27 MVPs available for the new performance year. This includes six new MVPs:
- Diagnostic Radiology (MVP ID: M1498)
- Interventional Radiology (MVP ID: M1499)
- Neuropsychology (MVP ID: M1500)
- Pathology (MVP ID: M1501)
- Podiatry (MVP ID: M1502)
- Vascular Surgery (MVP ID: M1503)
A full list of MVPs can be found here.