
During the National Association of Accountable Care Organizations (NAACOS) 2023 Spring Conference, the Centers for Medicare & Medicaid Services (CMS) highlighted its ambitious plan for transitioning fully to digital quality measurement. Their focus is on improving healthcare quality, aligning with the CMS Quality Strategy, reducing the burden on healthcare providers, and promoting health equity. In this blog post, we will discuss the CMS digital quality measurement transformation goals, Accountable Care Organization (ACO) engagement efforts, and lessons learned from these initiatives.
Digital Quality Measurement Goals
Quality measurement has undergone significant changes over the years from conventional paper-based methods (e.g., data from claims and manual chart extraction) to electronic clinical quality measures (eCQMs) that utilize data from electronic health records (EHRs). CMS is now committed to enhancing quality measurement by transitioning to digital quality measures (dQMs). Digital quality measures can incorporate various data sources beyond the EHR to streamline the quality measurement process.
The CMS dQM Strategic Roadmap provides a comprehensive framework to shift all quality measures to dQMs within its reporting programs in the coming years. The agency recognizes that healthcare providers and care settings have varying levels of preparedness, and the timing of dQM implementation within different quality reporting programs may differ.
CMS defines dQMs as:
- Utilizing standardized, digital data from multiple sources of health information.
- Applying quality measure specifications that are standards-based and use code packages.
- Computing measures in an integrated environment without additional effort.
- Improving patient care and experiences by ensuring timely access to necessary information (rapid-cycle feedback).
According to the CMS Strategic Roadmap, future dQMs will query the data needed (for example, from Fast Healthcare Interoperability Resources (FHIR) Application Programming Interfaces (APIs)), calculate the measure score, and generate the required reports.
National Quality Strategy Goals
The CMS dQM Strategic Roadmap also aligns with the goals of the CMS National Healthcare Quality Strategy which emphasizes a patient-centered approach throughout the entire spectrum of care, from birth to end of life. The National Healthcare Quality Strategy consists of four priority areas and each area includes two specific goals with defined objectives and targets to ensure effective implementation.
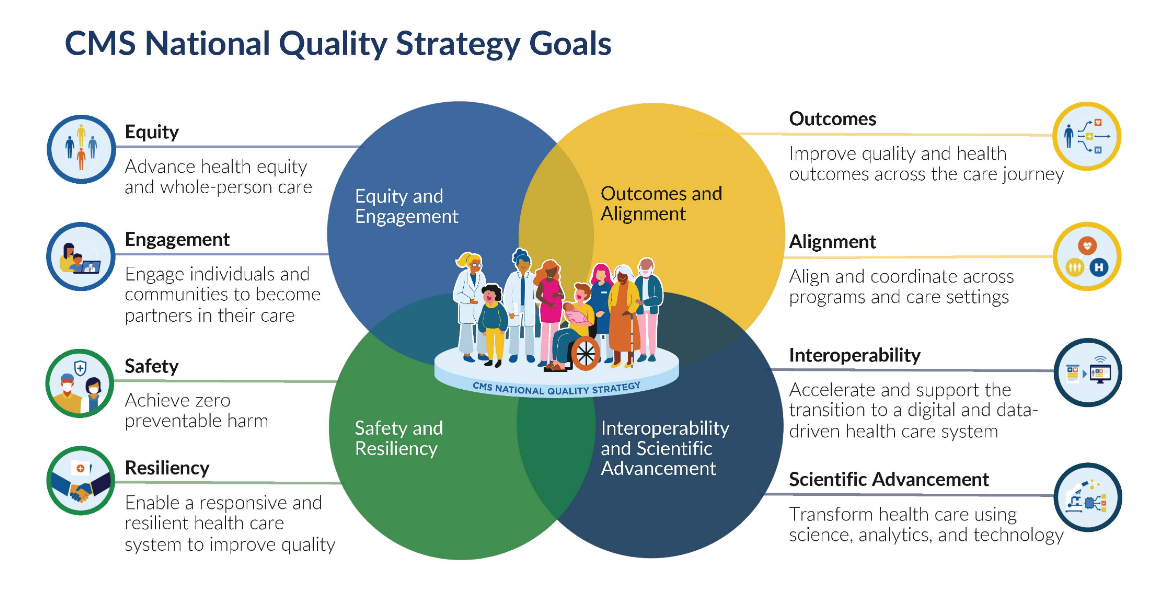
Image Source: CMS National Quality Strategy
ACO Engagement Efforts and Reporting Options
As part of these efforts to enhance quality measurement, CMS is implementing program-wide requirements for digital quality measurement in the Medicare Shared Savings Program (MSSP). To support ACOs in their transition to digital quality measurement, CMS has provided two reporting options for ACOs through 2024. ACOs can either report three eCQMs/MIPS CQMs and administer the CAHPS for MIPS Survey or report ten CMS Web Interface measures and administer the CAHPS for MIPS Survey. In both options, CMS will automatically calculate and score ACOs on two administrative claims-based measures included in the APM Performance Pathway (APP). Starting in 2025, ACOs will have to use eCQMs and dQMs for their quality reporting in the APP.
Timothy Jackson, Director Division of Quality and Price Transparency at CMS, emphasized a key point during his presentation at the NAACOS conference: "On March 31, 2025, the web interface will close and it will never open again." This statement underscores the importance of staying ahead of the curve and adapting to the changing landscape of healthcare reporting.
Lessons Learned and Best Practices
CMS has learned valuable lessons from ACOs' eCQM and MIPS CQM reporting experiences. These lessons can be applied more broadly to improve healthcare data interoperability and support a successful learning health system. Some of the critical aspects of successful eCQM/CQM reporting include patient matching, data deduplication, data completeness, and data aggregation.
CMS is also exploring necessary tooling and infrastructure to support patient matching and data de-duplication. These efforts include:
- Conducting User Experience (UX) Interviews with ACOs and industry groups
- Planning for prototyping Bulk FHIR Client tooling, and experimenting with FHIR data storage infrastructure to pilot with early adopter ACOs
It is worth noting that there has been progress in the reporting of eCQMs/CQMs measures by ACOs. In 2021, 12 ACOs successfully reported the 3 eCQMs/CQMs measures, and this number increased to 37 ACOs in 2022. This demonstrates the growing adoption and success of ACOs in implementing digital quality measurement strategies.
What ACOs Are Saying
Different ACOs also shared their experiences with collecting data from disparate EHRs, or even from providers without certified EHRs or those still using paper records, during the NAACOS conference. EHRs can produce QRDA files that are difficult to process because some EHR vendors have variations in their implementation of the QRDA standard. One ACO shared their experience of moving to FHIR to bypass the QRDA process and establish a more live interfacing with their different practices. This approach enables more efficient data exchange and promotes greater interoperability across healthcare systems.
How MDinteractive Can Help
Our MDinteractive registry has extensive experience with the types of issues that ACOs face when aggregating data from various sources. We are using FHIR to speed up the reporting process and effectively address data aggregation challenges. MDinteractive’s expertise can help ACOs overcome the hurdles in collecting, processing, and reporting data, ultimately contributing to the overall goal of improving healthcare quality and outcomes.
ACOs are continuously learning and adapting to the challenges of collecting and aggregating data from multiple sources, including disparate EHRs and paper records. By utilizing technologies like FHIR and collaborating with experienced registries like MDinteractive, ACOs can streamline their reporting process and enhance interoperability across healthcare systems.
Looking Forward
As the CMS Web Interface is set to close in 2025, ACOs must continue to adapt and stay ahead of the curve. The lessons learned from ACO engagement efforts provide valuable insights for broader healthcare data interoperability and the development of a successful learning health system. As CMS continues to work towards achieving its National Quality Strategy Goals, it will be essential to engage with experienced registry vendors like MDinteractive and deploy as soon as possible the necessary tooling and infrastructure to support these initiatives.
Schedule a meeting to learn more about how MDinteractive can help your ACO successfully navigate APP reporting.